Suppression
Prior to the execution of the NetworX adjudication module, claims may first pass through third party clinical editing and/or editing/auditing native to the SCE. If specific claim lines are denied due to an editing process, those identified lines are automatically suppressed, or withheld from inclusion in the API call to NetworX.
The table below represents 3 scenarios in which claim lines are suppressed following claim line denial recommendations: (a) a single line claim with single claim line denial, (b) a multiple line claim, with all lines denied, and (c) a multiple line claim with multiple, but not all lines denied.
In these scenarios, the denied claim lines are suppressed and withheld from the request XML file transferred to NetworX, and upon the return of pricing data from the NetworX XML response file, all claim lines are merged back together before continuing in the adjudication process.
The denial recommendations are identified with discrete event codes in the system, and the presence of those event codes on the suppression configuration table enables the line to be denied. This model allows you to add other event codes to the suppression.
| Scenario | Action |
| Single line claim - line denied | Suppress entire claim |
| Multiple line claim – all lines denied | Suppress entire claim |
| Multiple line claim – all lines NOT denied | Suppress denied claim lines – do not send suppressed lines to NetworX |
NetworX claim line suppression rules are configured in the SANPClaimLineSuppression
decision table shown below. 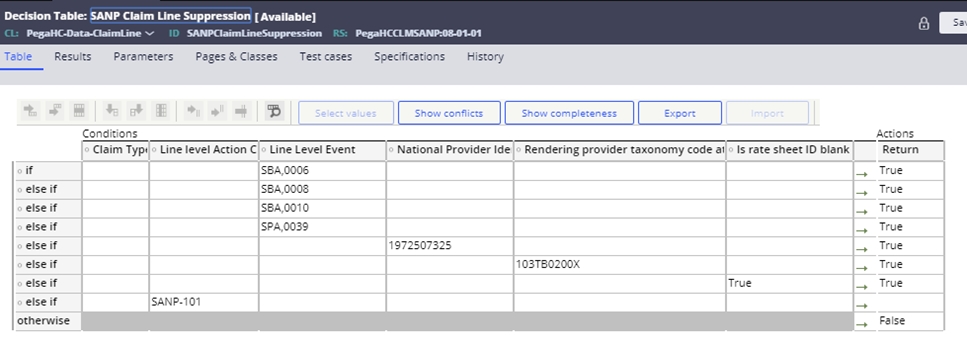
Note: this decision table can also support the configuration of other attributes used for suppression, such as claim types (institutional vs. professional), action codes, NPI, provider taxonomy, and the presence/absence of rate sheets.
Previous topic NetworX integration points Next topic Mapping claims objects
