Overview
Pega’s Smart Claims Engine (SCE) is an application that addresses the complexities of healthcare core claims administration by providing a flexible platform solving a wide variety of business challenges and supporting multiple integration models. At the heart of the solution is an orchestration platform and a robust claims data model that enables different modules to be executed based on the business problem and functionality that is being implemented. The SCE also provides a robust user interface to configure various processing rules and support the adjudication, resolution, and administration of claims.
The SCE sits on top of the Pega Infinity™ platform and the Pega Foundation for
Healthcare and can integrate with external point solutions, client claim processing
systems, and the other Pega healthcare applications. 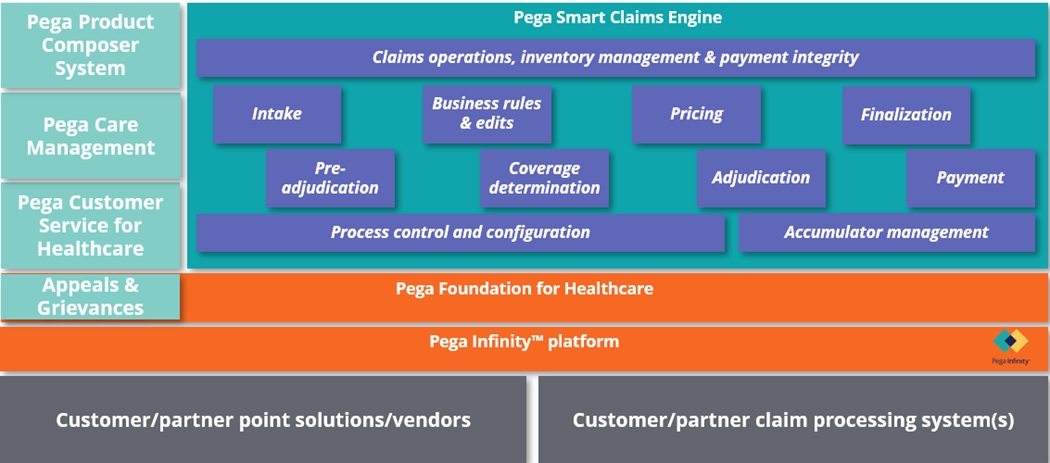
Smart Claims Engine includes an orchestration layer that calls discrete modules, each of which provides the business logic needed to successfully, accurately, and completely adjudicate a claim. The business logic is purposely modular to integrate either with relevant Pega applications or your organization’s solution. Smart Claims Engine provides a high-performance processing environment and enables payers to leverage their existing subsystems and capabilities, along with other vendor solutions.
Pega’s situational layer cake architecture and module-driven design enable the creation of business processing, validation, and edit rules. You can specialize these rules by any number of variables such as geography, line of business, product type, claim type, and so on. The system generates high-performance compiled code from the models to optimize performance and automation.
Smart Claims Engine uses the Pega Foundation for Healthcare, which contains a rich set of standards-based healthcare data models such as X12, HL7, ICD, and HIPAA compliance rules. This layer functions as the backbone of the system and enables integration with other systems.
The diagram below
shows a high-level example view of the flow of claims, running through a series of
modules in the SCE and the supporting integration to an external adjudication
platform. 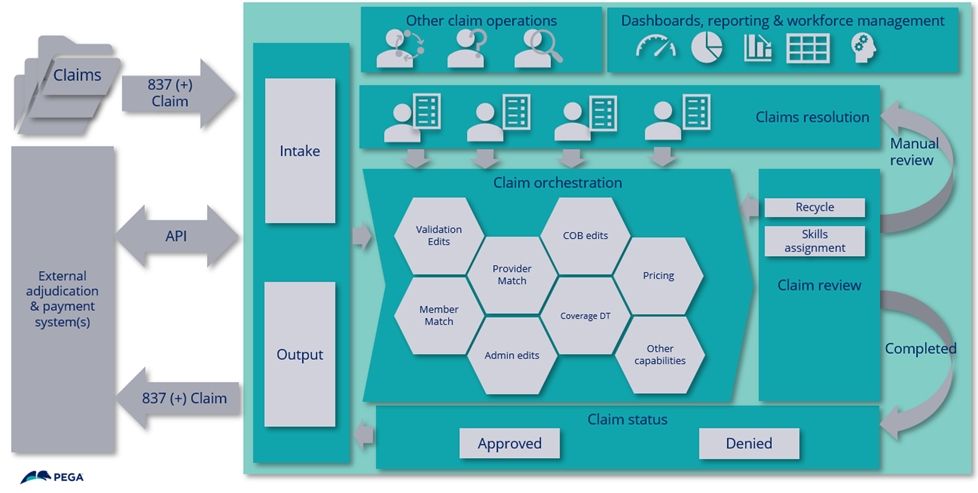
Once a claim comes in through the organization’s gateway and is pulled into our intake process, it runs through a sequence of orchestrated modules. Payers may uniquely configure processing steps and sequences, as well as the timing and application of pends, edits, audits, and override steps. Once finalized, claims are packaged and exported to your financial system by a batch process running on a periodic basis you choose.
Although the objective is to increase and sustain market-leading auto adjudication rates, Pega understands that healthcare payers can always have intentionally pended claims, either for audit, training review, or other business reasons. For that reason, Smart Claims Engine also includes an integrated pend resolution solution supporting end-to-end claims management.
Previous topic Purpose of the guide Next topic Key features of Smart Claims Engine
